Surgeons at the Orbital Surgery Center of Excellence in Los Angeles explain a new study regarding a common complication of hyperthyroidism and explain the benefits of a multidisciplinary treatment approach
According to a recent study published by the Department of Ophthalmology at New York Presbyterian Hospital, prominent cheek swelling in females may be indicative of thyroid-associated orbitopathy, also known as thyroid eye disease or Grave’s disease.
At the Orbital Surgery Center of Excellence, a sub-division of La Peer Health Systems in Beverly Hills, a renowned team of ophthalmologists, facial plastic surgeons, and otolaryngologists work together to treat a variety of complex orbital conditions. Mehryar (Ray) Taban, MD, FACS, believes that thyroid eye disease – which involves multiple organs – is best managed by a team of specialists.
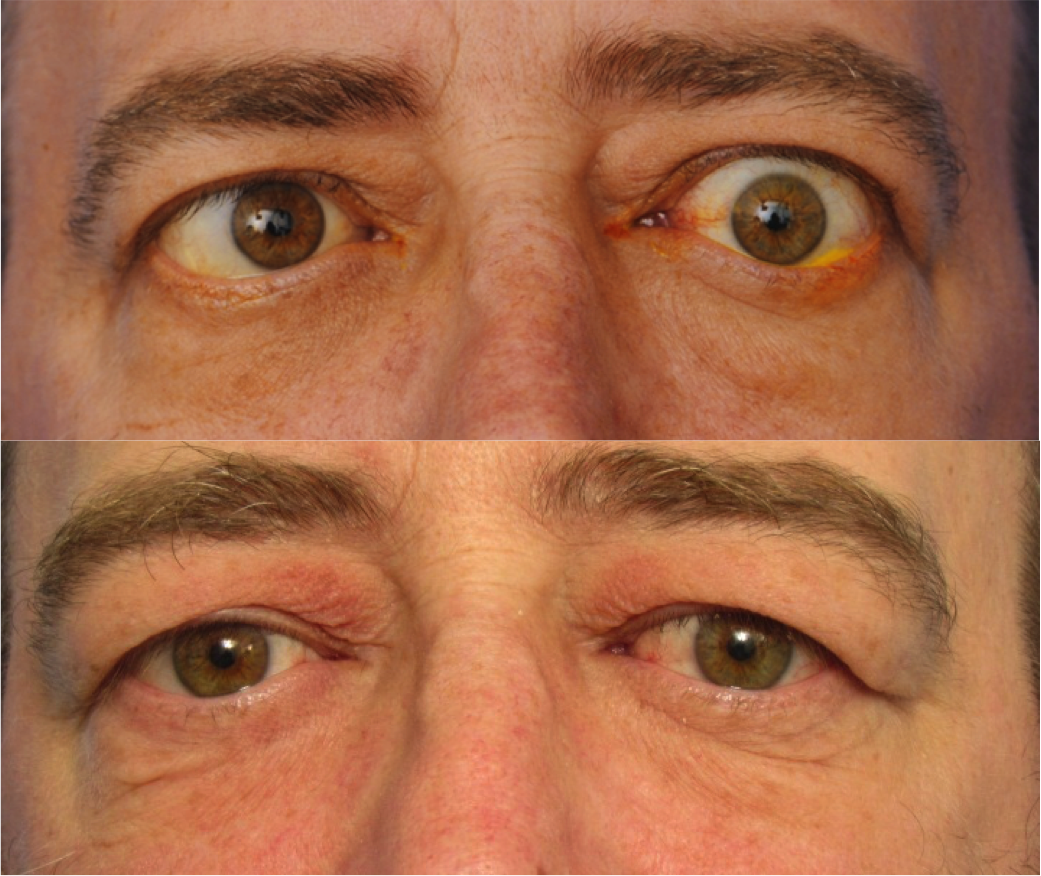
“Grave’s disease is the result of hyperthyroidism, in which an overactive thyroid gland produces an excess of hormones,” said Dr. Taban, the Medical Director at the Center of Excellence. “This may lead to a number of unpleasant symptoms, including insomnia, irritability, joint pain, and weight loss. But the most prominent symptom — which often requires surgery to resolve — is swelling and thickening of tissue behind and around the eyes, which can make the eyes and cheeks appear to bulge outwards.”
The study examined six female patients who experienced cheek swelling on both sides of their face and thyroid-associated orbitopathy. Of these six subjects, five were diagnosed with hyperthyroidism, which leads to Grave’s disease. It was determined that the sixth patient had an unrelated inflammatory autoimmune disease. Upon receiving treatment for their condition, cheek swelling improved in all patients.
Doctors at the Orbital Surgery Center of Excellence urge patients to seek treatment if they believe they could be suffering from a thyroid-related disease. Though not every case requires surgery, delayed treatment can increase the risk of severe orbital complications.
“In cases of Grave’s disease, a patient might need an otolaryngologist to treat the thyroid gland, an ophthalmologist to address any complications involving the eyes, and an oculoplastic surgeon to ensure appropriate facial balance following orbital decompression,” said Dr. David Savar, ophthalmologist at the Orbital Surgery Center of Excellence. “With a multi-disciplinary team of specialists, each surgeon can contribute their expertise to a certain aspect of treatment, thus ensuring the best possible outcomes for our patients.”
To learn more about the Orbital Surgery Center of Excellence, contact us today at (888) 559-4341.